What Makes Hip Fractures So Dangerous for the Elderly?
Every year, about 300,000 Americans experience a hip fracture.1 A hip fracture is difficult to recover from, in part because most patients are over 65 years of age.1 Unfortunately, the preliminary injury can lead to a significant decline in personal independence.1
A hip fracture is a break in the upper portion of the femur (thigh) bone. In the older population, it usually occurs due to falls (>95% of cases).1,2 Women account for around three-quarters of hip fracture cases.2
A hip fracture is a serious injury that can lead to lifelong impairment or even death. The one-year mortality rate for individuals who experience a hip fracture is 24%, and the likelihood of fatality increases with age.3 Among those who survive, under 50% ever return to pre-fracture functionality.3 They are also at increased risk of depression, delirium, dementia, morbidity, and subsequent fractures.3,4
Risk Factors for Hip Fractures
Aside from advanced age, there are various conditions that lead to an increased risk of suffering a hip fracture. These include the following:
● Osteoporosis: Weakens bones, making them more susceptible to fractures even with minimal trauma. This is a common condition that affects one of five women over age 50; additional risk factors for osteoporosis include physical inactivity, smoking, heavy alcohol use, low BMI (body mass index), and family history of the disease.5
● Gender: Women are more likely to suffer from osteoporosis, increasing their risk of this type of injury.6
● Falls: The primary cause of hip fractures; individuals with a history of falls are at a higher risk.2
● Poor Nutrition: Deficiencies in calcium and vitamin D can lead to weakened bones and a higher likelihood of a broken hip in elderly persons.6
● Medications: Certain medications can affect balance, increasing the risk of a broken or fractured hip bone.6
● Physical Inactivity: Lack of regular exercise contributes to weaker muscles and bones, heightening the risk of hip fractures.6
● Visual Impairments: Poor vision can lead to falls and subsequently to hip fractures.6
● Chronic Medical Conditions: Conditions such as cardiac conditions, Alzheimer’s disease, Parkinson's disease, multiple sclerosis, and arthritis can impair balance and coordination, increasing the risk of falls and broken hips.2,6
● Bone Cancer: Increases the likelihood of weakened bones, making them more susceptible to fractures.2
● Environmental Hazards: Cluttered living spaces, poor lighting, and lack of safety equipment like handrails and grab bars can contribute to falls and subsequent hip injury.6
How Hip Fractures Happen
Hip fractures among the elderly primarily occur due to falls. These falls can result from a variety of situations, such as tripping over an object, slipping on a wet or uneven surface, or losing balance while walking or standing. The impact from a fall can cause the femur to break, commonly referred to as a hip fracture.1
Another significant cause of hip fractures is high velocity trauma to the hip area. This can happen during car accidents or other high-velocity events. Although less common in the elderly due to generally lower activity levels, such traumatic incidents can still occur and result in severe fractures. The force of the impact from a high velocity injury affects the femur, leading to a break that requires surgical intervention.1
In some cases, hip fractures can happen without a fall or significant trauma. This is particularly true in individuals with severe osteoporosis, where the bones are so weakened that even simple actions like twisting the leg awkwardly, standing up from a chair, turning in bed, or even coughing can lead to a fracture, usually in the femoral neck.1,5
Stress fractures are another type of hip fracture that can occur without a significant fall or trauma. These fractures are small cracks in the bone that develop over time due to repetitive stress or overuse. They are more common in athletes but can also occur in older adults with osteoporosis. Stress fractures can lead to a full fracture if not properly managed and treated.1
Types of Hip Fractures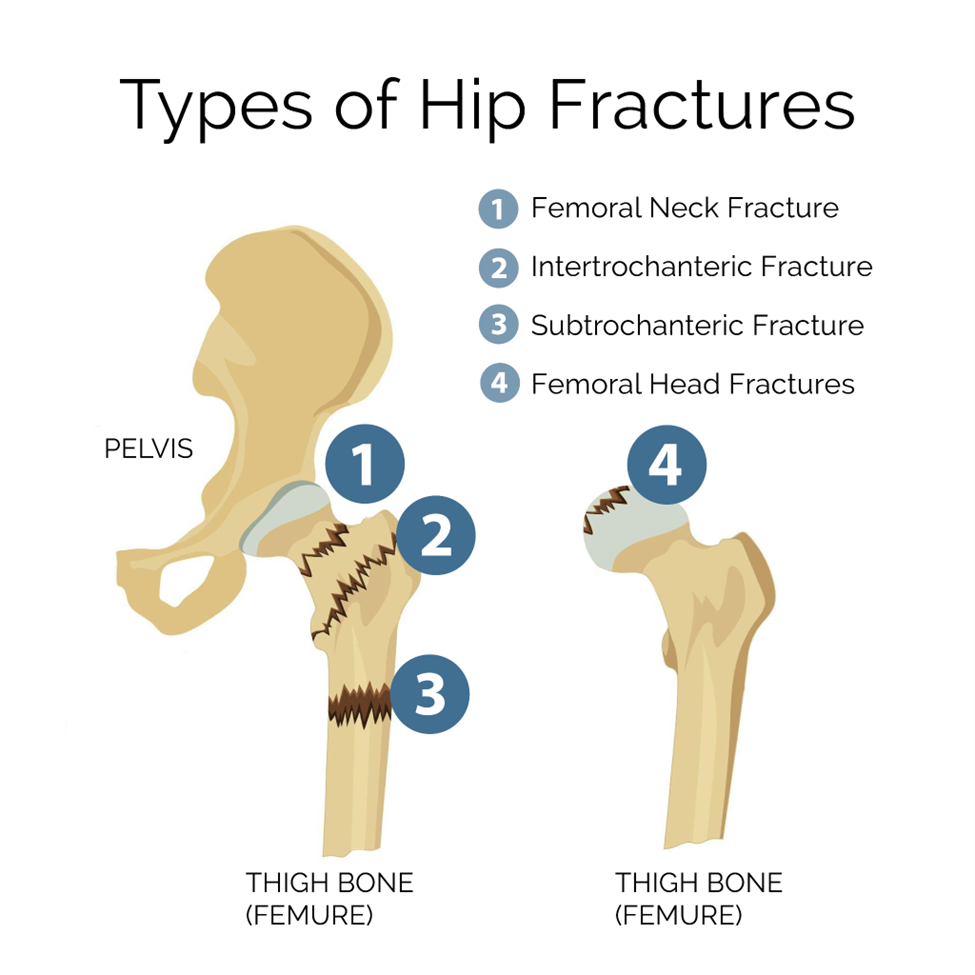
There are four areas of the hip where a fracture can occur:
Femoral Neck Fractures - These occur just below the ball of the ball-and-socket hip joint. They are common in older adults and can disrupt the blood supply to the femoral head.
Intertrochanteric Fractures - These occur between the neck of the femur and a lower bony prominence called the lesser trochanter.
Subtrochanteric Fractures - These occur below the lesser trochanter, in the upper part of the femur's shaft.
Femoral Head Fractures - These rarely seen fractures occur at the top of the femur and often involve a dislocation of the hip joint.1
Symptoms of Hip Fracture
Hip fracture symptoms typically include severe pain in the hip or groin area, which intensifies when trying to move, stand, or walk. Furthermore, the hip area may become stiff, swollen, and bruised. Another telltale sign is the appearance of the leg on the injured side, which may look shorter and turn outward.1
Can You Walk with a Fractured Hip?
Walking with a fractured hip is usually not possible due to the severe pain and instability caused by the break. Hip fractures lead to intense pain in the hip or groin area, especially when trying to move, stand, or walk. Immediate medical attention, usually requiring surgical intervention to stabilize the fracture is needed.1
Recovering from Hip Fracture

Making a full recovery from a hip fracture is a multi-step process. The vast majority of hip fracture patients will require surgery, typically within 1-2 days after the injury occurs.1,3 Following surgery, care must be taken to ensure a proper recovery.
Surgical Options
Treatment of a hip fracture is determined based on the type and location of the fracture, the patient's overall health, and the surgeon's expertise. Each method aims to stabilize the fracture and restore mobility as far as possible.7 Surgical Options include:
● Total Hip Arthroplasty
○ Involves replacing both the femoral head and the acetabulum (hip socket) with prosthetic components. This type of broken hip treatment is often used for severe fractures or in cases where the hip joint is damaged by arthritis.
● Hemiarthroplasty
○ Only the femoral head is replaced with a prosthetic implant. This procedure is often recommended for fractures that occur in the femoral neck.
● Long Cephalomedullary Nails
○ These nails extend down the femoral shaft and are used to stabilize intertrochanteric and subtrochanteric fractures. They provide strong internal fixation and are suitable for complex fractures.
● Short Cephalomedullary Nails
○ Similar to long nails but shorter in length, these are used for intertrochanteric fractures. They offer less invasive stabilization and are appropriate for less complex fractures.
● Sliding Hip Screw ± Anti-Rotation Screw
○ This method involves inserting a screw into the femoral head and securing it with a plate along the femoral shaft. An anti-rotation screw can be added to prevent the femoral head from rotating, which provides additional stability for intertrochanteric fractures.
● Multiple Screw Fixation
○ Utilizes several screws to stabilize the fracture site. This technique is often used for femoral neck fractures where the bone fragments are well aligned. It is a less invasive option compared to total or partial hip replacement.
Post-Surgery Recovery
Recovering from hip fracture surgery typically involves several steps:
Initial Recovery Phase
Post-surgical recovery begins in the hospital, where the initial focus is on managing pain and preventing potentially severe complications such as blood clots, infections, deconditioning and pneumonia. Early mobilization is crucial to facilitate healing and prevent stiffness. Patients are encouraged to begin physical therapy as soon as possible, often within a day after broken hip surgery.1
Rehabilitation
Physical therapy plays a vital role in broken hip recovery. Some patients will need to enter a acute short-term rehabilitation facility, while others will be able to go directly home. Occupational therapy may also be included to help patients adapt to daily activities and ensure a safe home environment. Patients perform exercises to improve their strength and flexibility. If the patient receives fixation surgery, it will generally take several weeks before they can safely walk unassisted.1
Long-Term Recovery
Broken hip recovery time can take several months. Continued physical therapy helps in regaining full mobility and strength. Regular follow-up appointments with the healthcare provider are necessary to monitor progress and address any concerns. It is important to bear in mind that a return to full pre-injury functionality may not be possible.1
Preventing Hip Fractures
Hip fractures are a serious concern, particularly for older adults. Preventing these fractures usually involves a combination of lifestyle changes, home modifications, and medical management. By taking proactive steps, individuals can significantly reduce their risk of sustaining a hip fracture.
Maintain Bone Health
Ensuring strong bones is crucial in preventing hip fractures. This includes a diet rich in calcium and vitamin D. Dairy products, leafy green vegetables, and fortified foods are excellent sources of calcium. Vitamin D can be obtained from sunlight exposure, supplements, and foods like fatty fish. Regular exercises, such as walking and weight training***, help build and maintain bone density. It's important to avoid smoking and excessive alcohol consumption, as these can weaken bones over time.5,6
Home Safety Modifications
Creating a safe home environment can significantly reduce the risk of falls, a common cause of hip fractures. Key modifications include installing handrails on both sides of staircases, securing loose rugs, getting rid of throw rugs, and ensuring that walkways are clear of clutter. Adequate lighting in all rooms and hallways is essential, as poor visibility can increase the risk of tripping. In the bathroom, installing grab bars and using non-slip mats can help prevent falls.2,6
Regular Health Check-Ups
Regular medical check-ups are essential for preventing hip fractures. Bone density tests can help identify individuals at risk for osteoporosis, allowing for early intervention. Medications to strengthen bones may be prescribed by a healthcare provider. It is also important to review medications with a doctor, as some drugs can cause dizziness or affect balance. Vision and hearing tests can help ensure that sensory impairments do not contribute to falls.6
Exercise and Physical Activity
Engaging in regular physical activity improves muscle strength, coordination, and balance, all of which are important for preventing falls. Balance exercises, such as tai chi, can be particularly beneficial. Exercises should be tailored to the individual's abilities and limitations, and it may be helpful to consult a physical therapist for personalized recommendations.6
By adopting these preventive measures, individuals can greatly reduce their risk of hip fractures and maintain a higher quality of life.
Seek Treatment at Crystal Run Healthcare
 Our orthopedic surgeons specialize in the latest minimally invasive techniques that lead to less pain, scarring, and hip surgery complications. A faster recovery and a more favorable outcome are our goals. Our surgeons can perform a total hip replacement, anterior hip replacement, hip resurfacing, or hip arthroscopy. From diagnostic imaging to pain management and physical therapy, elderly patients with a broken hip can depend on us for the best care.
Our orthopedic surgeons specialize in the latest minimally invasive techniques that lead to less pain, scarring, and hip surgery complications. A faster recovery and a more favorable outcome are our goals. Our surgeons can perform a total hip replacement, anterior hip replacement, hip resurfacing, or hip arthroscopy. From diagnostic imaging to pain management and physical therapy, elderly patients with a broken hip can depend on us for the best care.
To learn more about Crystal Run Healthcare and find a hip specialist, contact us at 845-703-6999, submit your questions online, or request a callback today.
*** Disclaimer on Exercise
*** Talk with your doctor before significantly increasing your activity level. Ask about the amounts and types of activities that may be best for you. Remember, moderation is best when starting an exercise regimen. Start slowly and gradually increase how often, how vigorous and how long you exercise. Moving even a little improves your health.
Sources
- The American Academy of Orthopaedic Surgeons (AAOS). Hip Fractures, Updated 11/2020.Hip Fractures | OrthoInfo - AAOS, Accessed 7/3/2024
- The American Academy of Orthopaedic Surgeons (AAOS). Updated 6/2023. Guidelines for Preventing Falls, Accessed 7/3/2024

 Optum Radiology at Crystal Run Healthcare
Optum Radiology at Crystal Run Healthcare Same and next-day pediatric appointments
Same and next-day pediatric appointments